In any tonometer (based on today's technology), you can have some, but not all of, the following:
- ease of use
- accuracy (reliability and validity of data)
- low cost
- portability
 People tend to give a priority to portability and low cost. New products aimed at this feature set have recently been announced. Does it make sense to utilize those devices for self-tonometry?
People tend to give a priority to portability and low cost. New products aimed at this feature set have recently been announced. Does it make sense to utilize those devices for self-tonometry?
We have to agree that any trade off that doesn't include reliability and validity of IOP data invalidates the whole endeavor of self-tonometry. Not only is it meaningless to do it if the data is not of sufficient quality upon which to make important decisions, but it could actually be detrimental to do self-tonometry in that case.
With today's technologies, portability entails user-alignment (in the context of self-tonometry). Proper user-alignment to produce a valid measurement, by definition, depends upon user skill as well as various specific conditions of each measurement. User-alignment, regardless of the tonometer, is difficult! (User-alignment is defined as the operator of the tonometer having to align the tonometer with the eye manually. Alignment is a very precise process requiring a steady hand, good eyesight, training and practice.)
Therefore, the requirement of user-alignment conflicts with the requirement of reliability and validity of IOP data. We cannot guarantee reliability and validity of IOP data when variable user skills are required to produce that data.
If any decent ophthalmologist or scientist (or intelligent thinker) considers a set of IOP data, they must consider how the data was obtained. If patient skill played a critical role in producing that data, as it does when user-alignment is required, the clear thinking person will immediately discount that data. Therefore, the self-tonometrist's efforts may not produce much of value.

 We now know that intraocular pressure does respond to events in our lives, to our state of mind and emotions and to stress. However, before FitEyes came along in 2006 (and for several years afterwards) these facts were not recognized.
We now know that intraocular pressure does respond to events in our lives, to our state of mind and emotions and to stress. However, before FitEyes came along in 2006 (and for several years afterwards) these facts were not recognized. I learned about emotions and eye pressure, in part, by watching my favorite sports and measuring my eye pressure over a period of years. See
I learned about emotions and eye pressure, in part, by watching my favorite sports and measuring my eye pressure over a period of years. See  Results: NCX 125 elicited cGMP formation (EC50 = 3.8 ± 1.0 μM) in PC12 cells and exerted NO-dependent iNOS inhibition (IC50 = 55 ± 11 μM) in RAW 264.7 macrophages. NCX 125 lowered IOP to a greater extent compared with equimolar latanoprost in: (a) rabbit model of transient ocular hypertension (0.030% latanoprost, not effective; 0.039% NCX 125, ∆max = −10.6 ± 2.3 mm Hg), (b) ocular hypertensive glaucomatous dogs (0.030% latanoprost, ∆max= −6.7 ± 1.2 mm Hg; 0.039% NCX 125, ∆max = −9.1 ± 3.1 mm Hg), and (c) laser-induced ocular hypertensive non-human primates (0.10% latanoprost, ∆max = −11.9 ± 3.7 mm Hg, 0.13% NCX 125, ∆max = −16.7 ± 2.2 mm Hg). In pharmacokinetic studies, NCX 125 and latanoprost resulted in similar latanoprost-free acid exposure in anterior segment ocular tissues.
Results: NCX 125 elicited cGMP formation (EC50 = 3.8 ± 1.0 μM) in PC12 cells and exerted NO-dependent iNOS inhibition (IC50 = 55 ± 11 μM) in RAW 264.7 macrophages. NCX 125 lowered IOP to a greater extent compared with equimolar latanoprost in: (a) rabbit model of transient ocular hypertension (0.030% latanoprost, not effective; 0.039% NCX 125, ∆max = −10.6 ± 2.3 mm Hg), (b) ocular hypertensive glaucomatous dogs (0.030% latanoprost, ∆max= −6.7 ± 1.2 mm Hg; 0.039% NCX 125, ∆max = −9.1 ± 3.1 mm Hg), and (c) laser-induced ocular hypertensive non-human primates (0.10% latanoprost, ∆max = −11.9 ± 3.7 mm Hg, 0.13% NCX 125, ∆max = −16.7 ± 2.2 mm Hg). In pharmacokinetic studies, NCX 125 and latanoprost resulted in similar latanoprost-free acid exposure in anterior segment ocular tissues.
 ng things. I still enjoy efficiency. But sometimes it is more efficient to delay the next project's start and finish what was started rather than have to terminate it due to an artificial deadline and then pick it up again at a later time. I like going deep into things (whether discussions, research or building software) and having the time to do it well. And I have found that sometimes I even enjoy doing something in a completely inefficient manner (saying that still sounds sacrilegious). Sometimes I enjoy just plain being slow! (What have I just said! My gosh!)
ng things. I still enjoy efficiency. But sometimes it is more efficient to delay the next project's start and finish what was started rather than have to terminate it due to an artificial deadline and then pick it up again at a later time. I like going deep into things (whether discussions, research or building software) and having the time to do it well. And I have found that sometimes I even enjoy doing something in a completely inefficient manner (saying that still sounds sacrilegious). Sometimes I enjoy just plain being slow! (What have I just said! My gosh!) People tend to give a priority to portability and low cost. New products aimed at this feature set have recently been announced. Does it make sense to utilize those devices for self-tonometry?
People tend to give a priority to portability and low cost. New products aimed at this feature set have recently been announced. Does it make sense to utilize those devices for self-tonometry?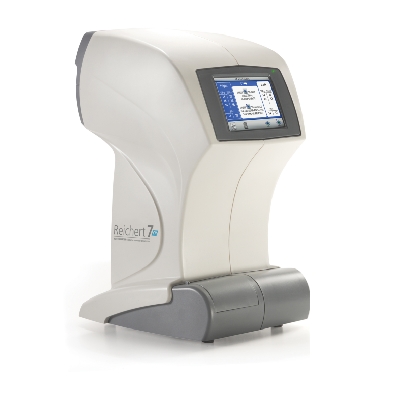 A lot of new people are joining our group for home eye pressure monitoring (self-tonometry). Please allow me to welcome all the new users and share a few thoughts about what to do when your new tonometer arrives.
A lot of new people are joining our group for home eye pressure monitoring (self-tonometry). Please allow me to welcome all the new users and share a few thoughts about what to do when your new tonometer arrives.