Help what should I do?
I just went to see my ophthalmologist yesterday and came away from the visit very worried. My pressure reading was 25 at first and then 21 after I put in a drop of Alphagan and Trusopt. The doctor said that even though pressure was high he still wanted to wait 3 months to see if it resulted in any damage to my nerves before deciding to give me the TCP laser procedure. However, I already have advanced glaucoma with considerable vision loss and do not wish to take the risk that I'll loss any more vision in the next three months.
- Read more about Help what should I do?
- kobo531's blog
- Log in or register to post comments

 This is the winning image for North America -- IN Cell Image Competition. It shows the internal structure of a single trabecular meshwork cell. In this image, DNA has been stained blue, so the large clumps of blue just above centre are the cell's nucleus. Red lines are filaments of actin spread throughout the cell, while the green patches at their tips are the focal adhesions.
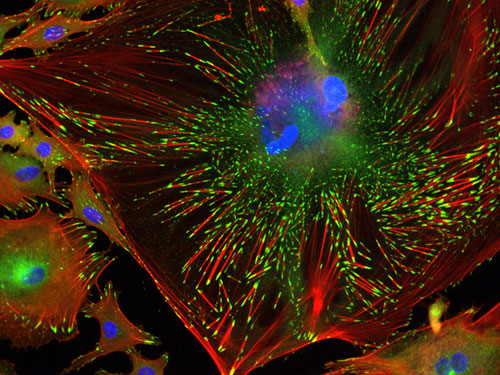
This is the winning image for North America -- IN Cell Image Competition. It shows the internal structure of a single trabecular meshwork cell. In this image, DNA has been stained blue, so the large clumps of blue just above centre are the cell's nucleus. Red lines are filaments of actin spread throughout the cell, while the green patches at their tips are the focal adhesions. This is from an email conversation between me and an ophthalmologist on the topic of research data.
This is from an email conversation between me and an ophthalmologist on the topic of research data.